- Home
- Advocacy
- Latest News and Practice Data
- December 7, 2021
December 7, 2021
In this Issue:
- Congress Explores Options to Address Medicare Cuts
- An Effort to Eliminate Federal Vaccine Mandate Fails in Senate, But Objections in the Courts Continue
- CAP Urges Administration to Revise No Surprises Act Regulation
- 2021 Practice Leader Survey Report: 1 in 5 Pathology Practice Have Consolidated
- Missed Our Final Medicare Payment Regulations Webinar? Watch the Recording
- Breaking Advocacy News: Check out the Advocacy Twitter Channel
Congress Explores Options to Address Medicare Cuts
On December 2, Congress passed legislation to avert a government shutdown and provide enough funding for federal programs through February 18. While the CAP and other physician associations lobbied lawmakers to use this funding bill to stop Medicare cuts in 2022, Congress neglected to do so. With little time left in the calendar year, congressional leaders are exploring options to address the cuts—including a vote in the House of Representatives later this week.
Mitigating the Medicare cuts has been a top priority for the CAP’s Advocacy throughout the year. The CAP and 10 other medical professional groups expressed disappointment in the fact Congress took no action on the cuts on December 2. At the same time, a strong, bipartisan majority in Congress support providing physicians with relief from the cuts and protecting Medicare beneficiary access to services. In addition, Congress has an historic record of stopping Medicare cuts to physicians for several years.
The CAP is tracking the pathways for Congress to address this issue. While it is preferrable that Congress pass legislation before the cuts are implemented, lawmakers may also retroactively mitigate the cuts later in 2022.
Finding a Legislative Vehicle
In years past, Congress has opted to include legislative language to stop or mitigate the Medicare cuts in larger legislative bills or omnibus packages. On December 6, House Majority Leader Steny Hoyer’s (D-MD) calendar indicated the House could vote on December 8 on several year-end business items, which included the Medicare cuts and raising the debt limit.
The Build Back Better bill, which Democrats hope to enact over the next several weeks, could also serve as a “legislative vehicle.”
Pass a Standalone Bill
Another option is for Congress to pass legislation introduced by Reps. Ami Bera, MD (D-CA) and Larry Bucshon, MD (R-IN). The bill is called the Supporting Medicare Providers Act of 2021. Sens. John Boozman (R-AR), Alex Padilla (D-CA), and Roger Marshall, MD, (R-KS) will be introducing legislation to provide the same relief in the Senate.
In December 2020, Congress passed legislation providing a 3.75% Medicare payment increase, which mitigated Medicare cuts due to budget neutrality requirements stemming from the Centers for Medicare & Medicaid Services’ policy to increase payment for evaluation and management services, for the 2021 Medicare Physician Fee Schedule and pausing budgetary sequestration cuts. The CAP has supported this relief be extended for another year. The Supporting Medicare Providers Act of 2021 would do just that by extending the 3.75% adjustment for an additional year.
Mitigating the Medicare Cut Retroactively
In the event Congress can’t address the cut by December 31, elected officials can opt to stop the cut retroactive to January 1, 2022. Congress has done this in previous years, including several times when Medicare’s sustainable growth rate (SGR) threatened steep decreases to physician reimbursement on a routine basis.
An Effort to Eliminate Federal Vaccine Mandate Fails in Senate, But Objections in the Courts Continue
Prior to the successful vote on the government funding bill, Senators on December 2 considered an amendment to eliminate the Biden Administration’s COVID-19 vaccination requirements on US businesses, the military, and the federal workforce. The amendment failed to gain a majority vote.
The CAP has supported requirements that direct large employers to ensure their workers are fully vaccinated or tested weekly for the coronavirus. The Biden Administration requires health care workers to get COVID-19 vaccinations by January 4, which is a mandate supported by the CAP and all of medicine.
CAP Joins Court Challenges in Support of Vaccine Requirements
Following the release of the new Occupational, Safety and Health Administration’s (OSHA) regulations for large employers, several business entities, states, and other organizations filed lawsuits to prevent the government from enforcing the rules. The plaintiffs contend the rules are an overreach of the OSHA’s authority, and they dispute the level of risk that COVID-19 presents to workers.
On December 1, the CAP joined an amicus brief in support of the requirements challenged in BST Holdings, LLC v. OSHA. The amicus brief is signed by other leading health professional groups, the American Public Health Association, and 100 educators, scholars, and public health professionals. The amicus brief contends that the plaintiffs have ignored the scientific evidence showing that workplaces are at risk for both transmission and infections with the coronavirus. The Biden Administration’s vaccine rule for large companies is based on the latest scientific evidence and would prevent thousands of hospitalizations and deaths from COVID-19, amicus brief states.
CAP Urges Administration to Revise No Surprises Act Regulation
In formal comments, the CAP urged the Biden Administration to revise the interim final rule for the No Surprises Act to align the law’s implementation with the original legislation. Specifically, the interim final rule for the independent dispute resolution (IDR) process disregarded Congress’s intentions to create a fair system where physicians and health insurers can resolve disputes without one factor having more weight over others in the final payment determination. The CAP strongly opposed the interim federal regulations that give insurance companies the upper hand during what should be an impartial, independent dispute resolution (IDR) process as set in the No Surprises Act.
In the December 6 letter to the Centers of Medicare & Medicaid Services (CMS), the CAP reinforced that the new regulations should protect patients from surprise bills “while appropriately balancing disputes between our members and insurers.” The CAP urged the CMS “to revise the decision to require the certified IDR entity to select the offer closest to the qualifying payment amount (QPA), and instead allow the authorized IDR entity to consider all relevant information thoroughly.” Especially in today’s environment, where “the majority of health insurance markets in the United States are highly concentrated, the CAP believes this decision is hugely problematic. “While it may take time to understand the full extent of resulting narrower networks, physician practice closures, and increased consolidation, these changes have the potential to decrease access to care for the most vulnerable, particularly in rural and underserved communities,” the CAP argued. Additionally, congressional champions pledged to intervene with the administration to clarify the intent of Congress and urge reform to the interim final regulation.
In the comment letter, the CAP also expressed their concerns regarding the good faith estimate requirements and the patient-provider dispute resolution process. Even though the CAP supports patient access to price information, the CAP argued to the CMS that “there are serious risks for patient harm and substantial difficulty in determining the cost of pathology services in advance of services.
The CAP will remain engaged with the administration to address the regulations and ensure they follow the statute.
2021 Practice Leader Survey Report: 1 in 5 Pathology Practice Have Consolidated
The CAP published the 2021 Practice Leaders Survey Report, providing the latest socioeconomic data on pathology practices’ structure and ownership status, case volume and revenue mix, practice staffing, and problems they incur with coverage and payment for services. In addition, the 2021 report reported on evidence of pathology practice consolidation.
According to the 2021 report, 10% of respondents indicated their practice acquired another practice/laboratory or group, and 6% merged with another organization or group. Additionally, 3% of respondents reported a portion of their practice/laboratory was acquired within two years. Together, these practices accounted for 19% of respondents, suggesting that nearly one in every five practices may have been involved in some type of practice consolidation in the last two years.
Organization and Structural Changes Affecting Practices Within the Last Two Years (n=304)
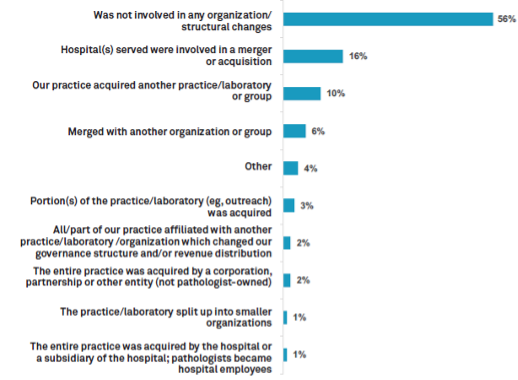
Source: Q36—Within the last two years, was your current practice/ laboratory involved in any of the following organizational/structural changes? (select all that apply)
Download the full 2021 Practice Leader Survey report (member login is required).
Missed Our Final Medicare Payment Regulations Webinar? Watch the Recording
Did you miss the final 2022 Medicare Payment Regulations Webinar? On December 3, the CAP hosted a webinar where experts reviewed the final regulation changes that will impact your pay, practice, and participation in the Merit-based Incentive Payment System (MIPS).
Missed the webinar? Check out the recording and download the slides.
Breaking Advocacy News: Check out the Advocacy Twitter Channel
Want up-to-the-minute CAP Advocacy news? Then follow us on twitter at CAPDCAdvocacy, where you will be the first to know about CAP Advocacy wins, see your fellow members engage with Congressional leaders on key policies affecting the practice of pathology and, of course, breaking Advocacy news.